Are you wondering how to treat eating disorders of all types with a single therapy approach.
You probably have heard a little bit about the 3 main types of recognized Eating Disorders – Anorexia Nervosa, Bulimia Nervosa, and Binge Eating Disorder.
Here’s a quick overview if you’re unfamiliar:
- Anorexia Nervosa is where someone rigidly restricts their food intake, doesn’t eat enough and generally speaking is dangerously underweight.
- Bulimia Nervosa is where someone again rigidly restricts their food, but then binge eats and purges their food out. People with this eating disorder often are at a normal weight because their restriction/purges cancel out the increased caloric intake from their binges.
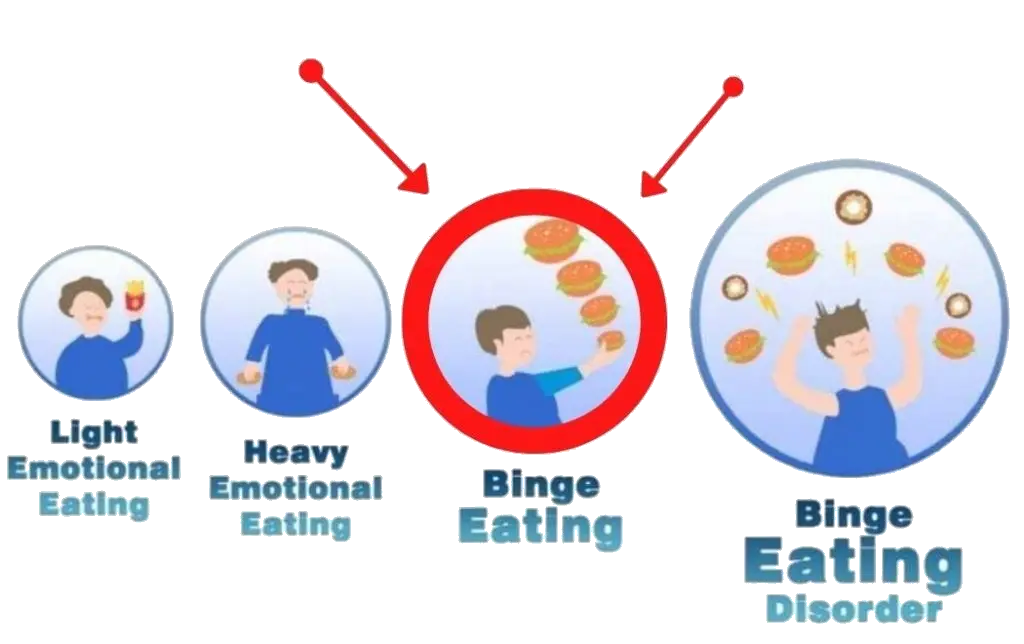
- Binge Eating Disorder is where someone binge eats but does not purge afterwards. People with binge eating disorder can be of normal size who restrict their foods (similar to Bulimia Nervosa) but many people who are obese have undiagnosed Binge Eating Disorder too.
You may think each of these 3 eating disorders requires a separate treatment, but in fact, Cognitive Behavioral Therapy can be used to treat eating disorders of all types.
That’s pretty cool, right?! I know you may be skeptical, but I just want to say that I am not a card-carrying CBT fanatic like some therapists are.
I’ll be honest too.
In looking at the Cognitive Behavioral Manual for Eating Disorders by Christopher Fairway, I’m feeling tremendously hopeful and inspired by his team’s idea of “transdiagnostic”.
This term means that there’s an underlying diagnosis behind all eating disorders, an idea that I believe is incredibly simplifying and which I’ll talk about near the end of the post more in depth.
In my experience with intuitive eating at an outpatient clinic as well as private private, people vacillate between restriction, compensation, binge eating and other symptoms.
By seeing all these symptoms as having an underlying set of causes, the person suffering can take specific aim at the underlying causes.
It’s like a house of cards, if you can target the underlying problems, then the whole thing will collapse.
In the same way, eating disorders all have a specific set of core pathology, or faulty beliefs. These perspectives are hidden underneath the restriction, obsession and binge eating.
Cognitive Behavioral Therapy gets at these core problems in a straightforward way which I really appreciate.
So this post will give two brief overviews of eating disorders and their causes, and then dive into how to treat eating disorders with cognitive behavioral therapy.
Specifically, in this post we will cover:
- What Are All The Types Of Eating Disorders?
- Brief Overview: What Causes Eating Disorders?
- Eating Disorders: How To Treat Using Cognitive Behavioral Therapy
- Why Cognitive Behavioral Therapy Treats All Types Of Eating Disorders
- Main Components Of Enhanced Cognitive Behavioral Therapy To Treat Eating Disorders
What Are All The Types Of Eating Disorders?
As you can see above, there are a ton of different eating disorders!
Trust me, I’m an eating disorder counselor and I still get a headache when I look at these different terminologies!
To make things even more confusing, many of these eating disorders have different subtypes.
For each of these, there are two subtypes with slightly different symptomatology.
Eating disorders are like a house of cards.
The different symptoms are like secondary and tertiary cards stacked at the top.
The foundation of the house of cards is built on the primary, structural eating disorder perspectives, behaviors and beliefs. As long as these primary issues can be seen, then the secondary mental health and treatment symptoms will take care of themselves.
Any type of therapy can target these underlying symptoms. In fact, family therapy I feel is sometimes more appropriate, especially if multiple family members are engaging in the eating disorder, which is not uncommon.
Even so, in this blog article I will just focus on Cognitive Behavioral Therapy (CBT).,
At this point it will help if we discuss the common origins of all Eating Disorders.
Brief Overview 2: What Causes Eating Disorders?
These are the causes of all types of eating disorders.
If we can tackle these problems, then the symptoms for all types of eating disorders can alleviate.
These are the root problems, the core struggles, that hold up the house of cards for all types of eating disorders.
I know this may seem like a tall order, but many of the above causes have a common cause at their core.
While problems like genetics we can do nothing about, notice that depression, anxiety, cultural issues, all of these have the similar problem of being in someone’s head!
So if we can help someone think differently, to see with a different perspective, to change their beliefs, …
Then the whole house of cards comes down, and that’s where we get into Cognitive Behavioral Therapy, which deals with ‘cognition’.
Eating Disorders: How To Treat Using Cognitive Behavioral Therapy
CBT is one of the most well-known research treatments.
There have been thousands of studies from different research universities, along with handbooks compiled by therapists in practice, all across the world.
The theory is proven over decades. It’s a hallmark of western medicine and treatment.
CBT helps with:
- Depression
- Addiction
- Mood Disorders
- Substance Abuse
- Psychotic Disorders
- Anxiety
- Anger Issues
- Low Self-Esteem
CBT can be applied in group settings and individual settings as well. It’s a really great form of therapy!
Now please notice that the types of problems that CBT works on, such as anxiety, depression, trauma, and low self-esteem), are some of the root causes of eating disorders too!
Plus, the basic principles of Cognitive Behavioral Therapy are easy to understand and measure from a scientific perspective.
It’s for these reasons that Cognitive Behavioral Therapy has such world-wide recognition. It’s of great help and easy to understand!
Basic Principles Of Cognitive Behavioral Therapy
Cognitive Behavioral Therapy is really simple to understand.
As a yoga teacher, meditator, and counselor, I really resonate with CBT’s simple approach, and I find the approach can help me out too in my life.
Our mind and body are one. Our thoughts impact our behaviors. This is the fundamental assumption of CBT.
For example, if a person with low self-esteem thinks ‘I am a total failure’, ideally they will challenge themselves or develop new skills. But in most cases they easily give up and don’t seek help.
By avoiding opportunities to develop new skills, or giving up prematurely, or by not seeking help, this person will miss out on conversations and be lonely, and conclude they are not worthwhile.
Yet if this person is able to shift their thinking from ‘I am a total failure’ to ‘I am learning a new skill and failure is part of the process and doesn’t mean I personally am a failure’, then they will be on the path to healing.
CBT can help. Here’s the basic diagram of CBT which shows how our thoughts and emotions impact our behaviors.
Why Cognitive Behavioral Therapy Treats All Types Of Eating Disorders
You might be wondering at this point what precisely makes Cognitive Behavioral Therapy suited for all types of eating disorders.
Let’s look at anxiety, which is one of the causal factors of eating disorders. At the same time, we know that anxiety is a factor in other situations that don’t involve eating disorders. .
For example, anxiety is a common factor behind a fear of public speaking or social situations.
And our initial thinking probably is that this fear of overcoming public speaking simply must have a different form of treatment when compared to binge eating.
So if CBT works as a treatment for anxiety then how could it also simultaneously work as a treatment for Eating Disorders?
Cognitive Behavioral Therapy Treatment For Eating Disorders
A hallmark of CBT-E disorder treatment is the concept of “transdiagnostic”, or going across diagnoses. This refers to treating eating disorders in the plural, rather than just a singular eating disorder.
CBT-E disorder treatment holds that the core problem underlying all eating disorders is the over-evaluation of body image, willpower, and perfection.
In essence, the over-evaluation of body image, perfection and control makes up the primary cards supporting the eating disorder house of cards.
If you can target, address, heal, get treatment for and ultimately integrate the over-evaluation of body image, perfection and control, then the rest of the eating disorder cards (the secondary and tertiary cards that I talked about earlier) will also come tumbling down.
For an example of what over-evaluation means, let’s take into consideration how people form their self-esteem.
A normal person derives their self-esteem from a variety of ways, such as family, friends, skills, community support, goals, overcoming setbacks, etc.
A person who has an over-evaluation of weight, control and body image might exclusively judge her self esteem if she lost weight that day.
She might have friends, family, skills, etc … But only eating, food and weight are what she bases her value on.
Because she only focuses on her weight, and food, this woman might skip family dinners. Or, she might stop caring about school or her relationships.
She might spend hours and hours exercising, counting calories, and looking at herself in the mirror.
All of this strange behavior comes from her seemingly insane over-evaluation of weight, body image and control.
And this type of core problem is extremely common!
For example, over 75% of 100+ clients that I have worked with individually have conscious or unconscious ideas of perfectionism and control.
In an extreme example, one woman believed that taking naps was a clear sign of ‘not-being productive’. In her attempts to always be productive, she missed out on many opportunities to take care of herself.
Trying to support 4 kids and a leadership marketing role at work is a tall order, and this woman was burning herself out. Her stress levels were incredibly high, and she was using food to cope with all of her stress.
To begin her treatment, instead of telling her to ‘just chill out’ or to find some downtime, we instead worked on her belief systems.
We discovered that she believed naps were truly evil.
But her belief about naps was previously unconscious, she wasn’t consciously thinking naps were truly evil, but in conversations with me it became clear that she did believe naps were evil.
However, when this woman consciously looked at the idea of napping, she could tell that naps were not truly evil. A half-hour nap never killed anybody!
So this woman was able to identify her faulty beliefs, and she even started taking some naps!
Her behavior changed as a result of her examining and questioning her beliefs.
At the Cielo House Eating Disorder out-patient clinics, I supervise clients who are extremely anxious and depressed about their weight, body image and their attempts at control.
(Interestingly, many of these clients are of normal weight, but because of their beliefs about weight they see themselves as incredibly obese)
The patients at Cielo House are out-patient, which means they exhibit high levels of severity. For this reason there are several people on a treatment team.
The treatment team at Cielo may include a doctor, dietitian, and nurse.
For severe eating disorder cases the additional treatment team members are necessary. This is because eating disorders can be fatal without eating disorder treatment and a treatment plan.
A person struggling with their mental health, along with a full-blown eating disorder, can need tremendous amounts of help. For example, the client may also have dangerously erratic heartbeats, and many of them before treatment may also be self inducing vomiting multiple times per day.
But whether you “just” have an aversion to naps, or exhibit more severe symptoms such as vomit multiple times a day, the underlying core root is still there – the over-evaluation of body image, perfection and control.
This over-evaluation of body image, perfection and control leads to the other symptoms found in eating disorders:
- Extreme dieting
- Binge eating
- Laxatives
- Excessive exercise
- Rigid diet rules
- Horrible body image
Overall, CBT-E disorder treatment is highly effective for the treatment of eating disorders.
As a national provider and leader in Eating Disorder Recovery, Eating Disorder Hope states that “CBT-E has also been a proven form of therapy for the treatment of eating disorders … as it includes educational components and the development of a meal plan. CBT is highly successful in that it addresses the psychological, familial, and societal facets correlated with eating disorders and directly focuses on the problematic thinking and behaviors that sustain eating disorder symptoms.”
Main Components Of Enhanced Cognitive Behavioral Therapy To Treat Eating Disorders
CBT-E is for the individual therapist or counselor in mind, like myself.
It has robust success rates, and honestly, one of the biggest reasons I stick with the Eating Disorder field is because of these success rates.
We can live normal, peaceful, even boring lives with food. But for so many people food has hijacked their life. and it doesn’t have to be that way.
Eating Disorder Treatment can truly lead to in life-changing results, relatively quickly. And with CBT-E disorder treatment, there’s plenty of evidence to back that up.
Over the years CBT-E has become very structured, 20 sessions to be precise. It’s meant to help people who struggle with all types of eating disorders.
(The exception is severe anorexia, where treatment can go 40 weeks)
The sessions are spread out across 4 distinct stages:
- Stage 1: Therapist and client meet 2x per week and the priority is understanding the patterns and finding stable eating patterns. There’s also education at this point about ‘survival’ mode which is what happens for many people with eating disorders.
- Stage 2: Depending on the client’s situation, additional targeted training modules and exercises are given to overcome specific challenges. Session frequency goes down to 1x per week.
- Stage 3: Weekly sessions are still in place, along with training on dealing with negative thoughts.
- Stage 4: Sessions are now bi-weekly as the client wraps up the program. Special emphasis is given to recovering from relapse at this point.
I’ll give a bit more info on each of these stages below too 🙂
Overall, please note that CBT-E places special emphasis on both mental health and the health professional. I’m especially talking about the bond between therapist and client.
We have to like each other basically! This is true for any eating disorder treatment plan.
CBT-E Stages
Stage 1:
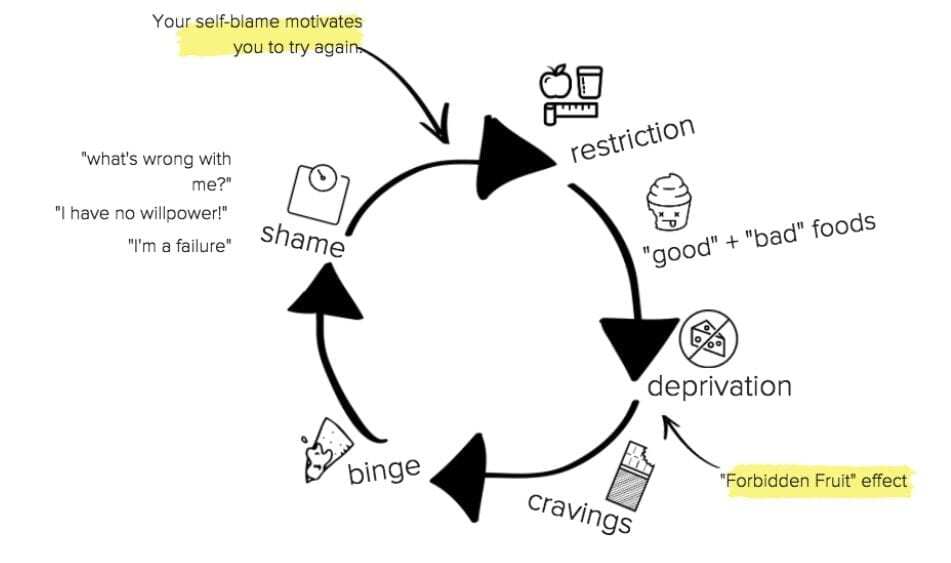
Understanding the core problem of restriction is paramount here in the beginning of eating disorder treatment. Therapist and client work together to create a personalized understanding of the cycle down below.
The job of the counselor is to help the client see this pattern for themselves, instead of just telling them, by asking open-ended questions.
In general this is how eating disorder treatment works best: the counselor (me) asks questions that help the client discover for themselves the underlying pattern.
The treatment plan can unfold more naturally this way, guided by the client’s own discovery about their mental health and what they need help on.
Stage 2:
The treatment programs shift to understanding the behaviors that keep the cycle intact. Now that the client has a better understanding of the cycle, they can begin to see this cycle in action.
The key is to shine awareness into the cycle at this point. To facilitate awareness, the client will be asked to study their eating patterns. Oftentimes a self-monitoring or reflection worksheet is given.
An essential part of this stage is journaling or some type of reflection.
The client needs to see for themselves the thoughts, emotions, triggers, results, patterns that lead to the pattern being repeated.
Stage 3:
At this point the topics relevant to all eating disorders have been covered with major patterns being explored and new habits and behaviors being utilized with success.
Depending on the person’s situation more training can be given to meal monitoring, behavioral trends, overcoming other barriers, challenging untrue thoughts.
Stage 4:
As CBT-E ends, special emphasis is given to relapse. The client’s new skills will greatly support relapse recovery.
In conclusion, CBT-E can be used to treat all types of eating disorders, some of which can be fatal if left untreated.
There are many people who can benefit from learning about these concepts.
There are solutions out there. The key now is to find a practicing professional and to simply start a conversation somehow.



Very nice article, exactly what I needed. Very useful post I really appreciate thanks for sharing such a nice post. Thanks
Thanks Andrew, there are many eating disorder solutions out there. I hope this articles helps, and the reader should know to continue searching out other eating disorder solutions as well!